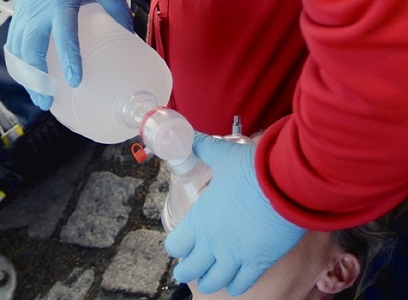
NTNU has been working to develop a nasal spray to reverse overdose for 10 years. The nasal spray has now been tested on 201 real overdose patients. Credit: Kai Eide/Oslo University Hospital
With a raging opioid epidemic, most stakeholders agree on the vital role naloxone plays in reducing opioid-related deaths. What they don’t necessarily agree on is the dosage and how the drug should be administered. Currently, recommendations range from 0.04 to 2.0 mg via the intravenous or intramuscular route. And while that administration has been proven to work, the popularity of nasal naloxone is on the rise due to ease-of-use.
Since 2015, several nasal naloxone products with single doses ranging from 0.9 to 8.0 mg have entered the market. These formulations were approved based on phase I pharmacokinetic studies in healthy volunteers alone—not the opioid-taking individuals who actually receive the drug.
“The lack of clinical trials of these high concentration/low volume sprays and the lack of trials comparing different naloxone regimens leave an important knowledge gap in best practice for management of opioid overdoses in the community,” a Norwegian research team explains in their new paper. “Clinicians, lay people, responders and policy makers should know precisely how a nasal naloxone spray performs in the field, compared to injectable antidotes. This requires studies that investigate both the effect and harm in the target population, allowing for evidence-based decision-making.”
The researchers’ study of 201 patients is the world's first trial of a commercially available and medically approved nasal naloxone spray in real cases of heroin overdose.
In the trial, participants treated by ambulance services for suspected opioid overdose were given a single dose (1.4 mg/0.1 mL) of naloxone nasal spray developed by researchers at the Norwegian University of Science and Technology (NTNU). Upon revival, they were asked if they were willing to participate in the trial, with 201 individuals consenting.
According to the trial results, 105 (97%) in the intramuscular group and 74 (80%) in the intranasal group returned to adequate spontaneous respiration within 10 minutes after one dose. The estimated risk difference was 18% in favor of the intramuscular group, while the risk of receiving a second dose of naloxone was 19% higher in the intranasal group. Adverse reactions were evenly distributed.
While a single dose of 1.4 mg intranasal naloxone was demonstrated to be inferior to 0.8 mg intramuscular naloxone, the overall findings show the nasal spray is still an incredibly effective antidote for those who overdose.
“It’s really encouraging that as little as a single dose of the nasal spray can restore breathing in 80 percent of overdoses. Nasal sprays can be given by anyone as first aid, even before the emergency services arrive. Friend overdose rescue is critical,” said co-author Arne Skulberg, a postdoctoral fellow at NTNU and anesthesiologist at Oslo University Hospital.
Skulberg and colleagues say their results indicate that the generally accepted 0.8 mg intramuscular naloxone dosage may be incorrect.
“Our findings that 0.8 mg [intramuscular] was sufficient for reversal in almost 100% of cases indicate that it was too high as a starting dose and lower doses should be tested,” write the study authors. “Pharmacokinetic trials show that dose-corrected concentrations of intravenous naloxone are many times as high as those achieved with intramuscular naloxone. This forms a strong argument for the efficacy and safety of the intramuscular route of administration in contrast to intravenous, which has a high probability of triggering withdrawal.”